A New Way to Manage Your Diagnosis
May 2022
The Benefits of Using a FHIR-Based Platform When Diagnosing Chronic Kidney Disease
Doctor Vivian Sing is an economics professor. She has a history of depression and diabetes, which she manages by exercising regularly and maintaining a healthy diet. A mother of three and grandmother of four, the 62-year-old prioritizes her health to ensure she can be there to celebrate her family’s milestones.
Then came the worldwide COVID-19 pandemic, shutting everything down. Gyms, restaurants and shopping malls were some of the first establishments ordered to close their doors. Everyone was being affected by the lockdowns. A study found that 27.8% of American adults felt elevated depressive symptoms within the first few months of the 2020 shutdown. This is compared to 8.5% prior to the pandemic. In 2021, that number rose to 32.8% of adults–thus tripling the depression rate within the US.
By having her routine thwarted, Vivian fell into this group. With gyms closed and no workout equipment at home, she found it extremely difficult to keep up with the exercise regimen essential to maintaining her mental health. Soon, like many other Americans, Vivian was unable to keep the depressive thoughts at bay. Eventually, finding the motivation to keep up with her diet also became difficult. What was once the occasional takeout meal being delivered to her home turned into a normal occurrence. Soon, Vivian struggled with being able to manage a healthy diet.
The negative changes to her lifestyle over the past year began affecting Vivian’s overall health and previous diagnoses. When her symptoms worsened, she knew it was time to see her doctor, where it was soon discovered that she had Stage 3 chronic kidney disease.
What makes Vivian’s case stand out from most other Americans in her position is the fact that her medical center has access to Smile Digital Health, an open standard data fabric enabled by Health Level 7 (HL7®) Fast Healthcare Interoperability Resources (FHIR®), that makes the patient’s data accessible from any application that is run on it. The medical center used the app PatientShare to find Vivian’s records and the app CareNexus to develop her treatment plan. PatientShare is a standards-based platform that enables secure clinical data to be seamlessly shared in order to enable collaboration among disconnected healthcare systems, while CareNexus is a coordinated treatment planning platform aiming to improve the quality of care and management of data among patients and providers across the continuum of care.
These integration platforms provide patients with a longitudinal health record allowing for a secure, private and transparent healthcare journey. Using appSphere—a productivity suite built into the Smile platform that makes connecting and managing third-party apps to Smile easy—a patient’s data can seamlessly be transferred among programs to ensure information is accurate and correct.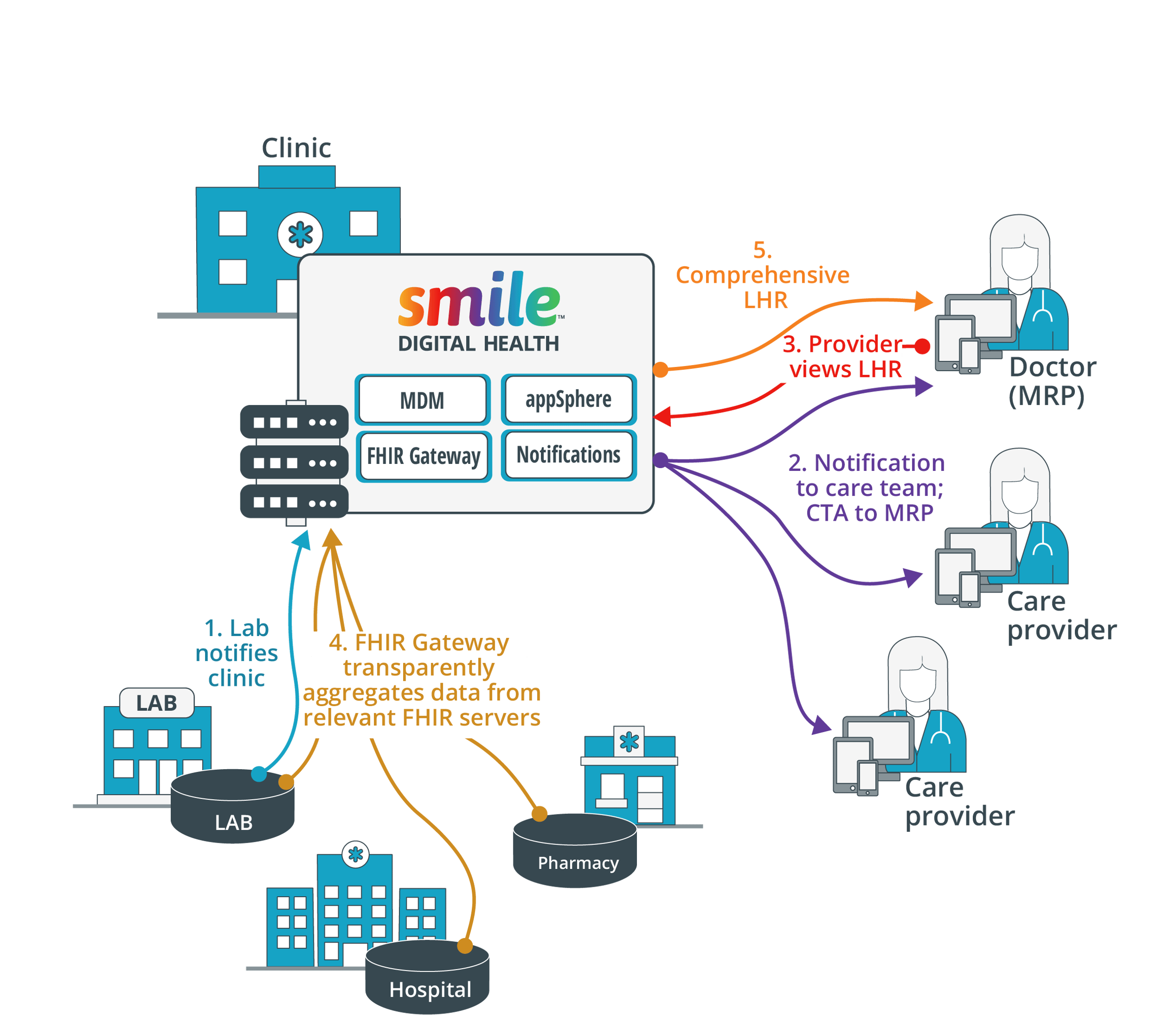
This standards-based solution employs HL7 FHIR APIs and allows for collaboration across disconnected healthcare systems. The great value of a FHIR-based platform is having actionable information accessible by the right people, shared securely in a timely fashion.
From a patient’s point of view, one of the biggest benefits of this software is empowering the patient to be an active partner in their own care, by being able to view their treatment plans and personal data and even to generate their own data. For a patient like Vivian it means no more missed requisitions, miscommunication between the doctor’s office and the specialist or any of the other important information overlooked due to healthcare’s resistance to technological advancements.
In Vivian’s case, Smile’s platform enabled her data to be accessible anywhere through the applications both she and her doctors used and can streamline a patient’s healthcare journey, from the first healthcare contact to treatment, without a delay in their diagnoses or personal care plan.
Because so many providers still rely on faxes and paperwork when updating patient information, most Americans experience a delay in their treatment. This is largely a result of the healthcare industry not adapting to new technologies that, when fully utilized, can benefit Providers and Payers alike. Until that happens across the board, discrepancies in patient care will continue.
If Vivian’s medical center wasn’t using a FHIR-based platform, the outcome could have been strikingly different. Thankfully, because both her primary care physician and nephrologist were able to update Vivian’s records in near real-time, she was able to receive her chronic kidney disease diagnosis while it was still in Stage 3.
A year of unhealthy diet habits and no exercise affected Vivan’s health. In addition to a low energy level, she noticed a slew of other physical symptoms including fatigue and mental fog, as well as swelling in her hands and feet and itchy skin. She gained weight and noticed increased depressive mood, however, without suicidal tendencies.
That’s when she decided it was time to get help.
Vivian made a quick phone call to schedule an appointment with her doctor. Luckily for her, the nurse at the centralized medical center was able to access her medical history through PatientShare, a secure data-sharing system.
The medical center nurse was able to confirm Vivian’s identity by verifying her Medical Record Number (MRN), as well as her date of birth and other personal information. From there, the nurse was able to view Vivian’s complete health records, including her current and previous diagnoses, medications and her most recent vitals. That’s how it was discovered that the last time Vivan had tests done was over a year ago.
How appSphere Stands Out
Vivian, like many others, previously struggled with incomplete health records, including lab results not properly being shared among her healthcare providers. Test results issued to her personal care practitioner’s (PCP’s) office often remained there, even when another doctor or specialist requested that information. With the two (or more) offices not effectively communicating with each other–as each only had part of Vivian’s healthcare record–she wasn’t always able to receive the best treatment.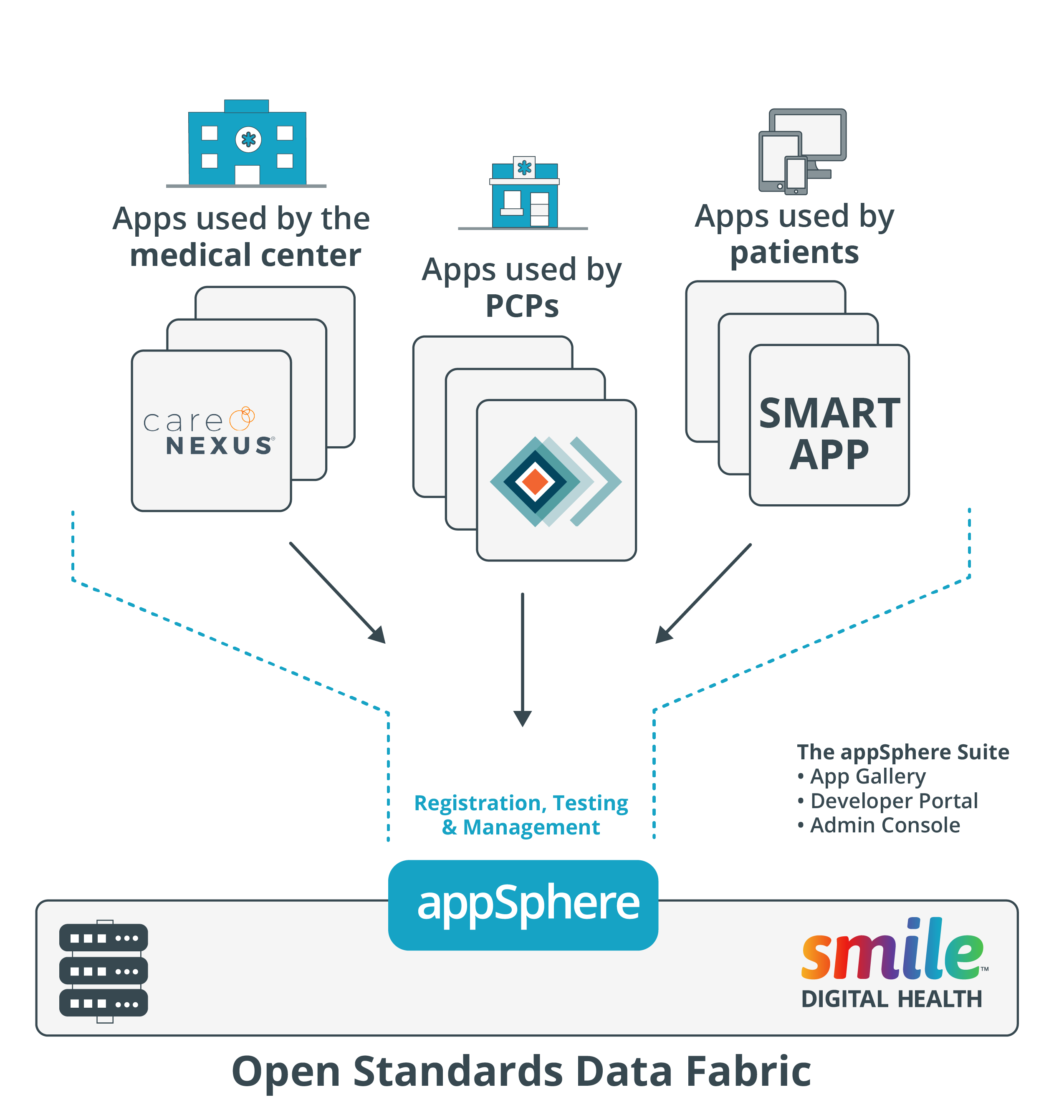 appSphere manages the entire application ecosystem and serves as the connector between patients, doctors, data and the application itself. Its gallery connects patients and doctors to their application of choice. The developer portal connects applications to the data and admin console connects the data to patients and doctors.
appSphere manages the entire application ecosystem and serves as the connector between patients, doctors, data and the application itself. Its gallery connects patients and doctors to their application of choice. The developer portal connects applications to the data and admin console connects the data to patients and doctors.
This enables healthcare workers to have access to multiple applications like PatientShare and CareNexus in order to access a patient’s electronic health record (EHR) and offer treatment solutions. This allows multiple care plan applications to connect with different FHIR servers, aggregating multiple results within the fragmented healthcare system. For patients like Vivian, this means that, despite seeing numerous doctors for various conditions, her healthcare records can be easily accessed by other physicians and even Vivian herself.
PatientShare allowed the nurse assisting Vivian to put in the request for updated blood work along with a follow-up the next month. The results from her blood work were immediately transferred to her PCP’s office, where it became clear that she needed an urgent consultation with a nephrologist in order to have her kidneys closely examined.
Based on the findings from Vivan’s tests, her PCP used CareNexus to add a health care plan to treat chronic kidney disease as well as a note to check-in with her in a week. By the time Vivian saw the nephrologist, her specialist was able to prescribe a low dose of antihypertensive and update the system with a more comprehensive Stage 3 chronic kidney disease care plan.
By using this FHIR-based platform, once Vivian’s lab results were ready, a notification was sent to her care team. Her Provider was then able to view Vivian’s Linked Health Resources (LHR) which can be seen by the lab, hospital and pharmacy through FHIR servers, at which point her nephrologist was able to prepare a comprehensive LHR.
Most people don’t have access to the same care as Vivian. The fact that she was able to receive a prompt, comprehensive treatment from the get-go is not yet the status quo. In fact, 90% of patients don’t actually know that they have kidney failure–the causes of which are usually preventable and can include diabetes or hypertension.
The added complexity in diagnosis is that acute kidney disease can also be a result of:
- An autoimmune disorder
- Certain medications
- Injury involving significant blood loss
- Heart or liver failure
There are plenty of reasons as to why so many people are unaware of their chronic kidney disease diagnosis. One of the biggest is age, as those over 60 are at a greater risk. Another important factor lies in delayed diagnosis resulting from late referrals and a late start to maintenance dialysis. A late referral could very possibly be the result of a person’s medical information not being easily accessible. It’s often trapped within siloed databases within the same healthcare center. If, by the time someone calls to make an appointment with their doctor, previous information on their medical history needs to be located by their PCP, it could take days before new tests are requested—and even longer for them to be completed. It goes without saying that the longer it takes for healthcare practitioners to file requisitions, the longer it takes for a diagnosis to be made.
The stages of chronic kidney disease are based on the glomerular filtration rate (GFR), which determines how well a person’s kidneys filter waste from their body. Determining the actual GFR takes a fair bit of time and money, which is complicated due to the already problem-ridden issue of diagnosing chronic kidney disease. Because of this, tests can be done to determine someone’s estimated glomerular filtration rate (eGFR) instead of measuring how well the kidneys are functioning. Though, as its name suggests, an eGFR is only an estimate, it’s much more cost-effective and significantly faster than a measured GFR while being nearly equally as reliable.
Using a FHIR-Based Platform to Determine Treatment Plans
What makes Vivian Sing’s case unique is the ease and timeliness of which she was able to receive care. Providers not using a FHIR-based platform don’t always immediately have the same access to patient records as Vivian’s medical center. Because of this, up to 50% of healthcare referrals are missed. For someone with chronic kidney disease, this could be the difference between a more manageable Stage 2 diagnosis or a worsened Stage 4 diagnosis.
During treatment, a patient with failing kidneys (Stage 4 or 5) needs dialysis three times per week, adding to the $120 billion annual cost in Medicare for those with kidney failure. If Vivian’s medical center was unable to access her records and electronically request that her tests be updated, she may have been part of that 50% who were unable to be tested in a timely manner, resulting in a late-stage diagnosis. The benefits of using tools like appSphere to access applications like PatientShare and CareNexus go beyond the ease of which Vivian’s medical center nurse was able to locate her and determine new tests were needed.
Once the results were available across the platforms, Vivian’s doctor was able to immediately request a nephrologist consult and add Vivian’s chronic kidney disease diagnosis to her file. As soon as her results were in, her doctors were able to create goals for Vivian’s treatment. This includes summarizing her condition, updating the status and progress (including whether or not a certain treatment is revoked and why) and setting a priority level and target date for completion. They also assembled a care team, specifying members and their roles. That way, Vivian’s treatment process could be viewed and updated by anyone with access to her plan.
By logging on, Vivian can also access her personal records and results. This gives her all the information she needs and can choose to share them with her loved ones, if desired. Not only does that allow her to know her treatment options, but she can be informed about how they can help navigate her Stage 3 kidney disease and work on managing her diagnosis.
Vivian’s treatment plan was clearly followed with secure, private and transparent features on a FHIR-based data and integration platform, powered by Smile, which uses high-level, multi-factor authentication operates to ensure that only approved users are able to access data, as a result of the integrated external identity providers.
At this time, seamless interoperability is possible. There have been so many advancements within healthcare technology that tools like appSphere, PatientShare and CareNexus, powered by Smile’s SMART on FHIR data platform, can be the new normal. The healthcare industry just needs to be open to change. Utilizing a FHIR-based solution will assist to bridge the current gaps in the healthcare system while transforming the health technology landscape. What this means for patients is a more timely, transparent, diagnosis and treatment options, better collaboration between their healthcare professionals, lower costs for healthcare systems, a reduced burden for Providers and an overall improved experience for caregivers and patients alike.
